Posted
27th March 2024
Research
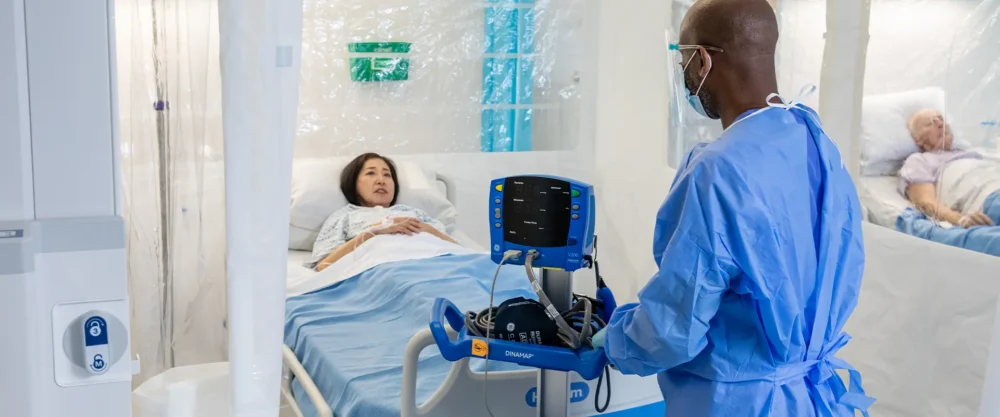
The importance of practising proper hand hygiene is widely considered to be the most effective means of preventing the spread of healthcare-associated infections (HAIs) and reducing contamination of the environment within healthcare settings1-2. With hand hygiene being a simple, yet effective way of preventing the transmission of pathogens, much emphasis has been placed on the role the healthcare worker plays in the transmission of HAI’s but it is important to note that patients’ and residents’ hands can also become contaminated and act as a source for spreading the infection.
It was shown that after admission into acute care, 39% of patients’ hands sampled were contaminated with at least one pathogen after just 48 hours3, whilst another study showed that 75% of aged care residents’ hands were contaminated with potentially harmful pathogens4. These harmful pathogens included, Clostridioides difficile, Staphylococcus aureus (MRSA), vancomycin-resistant enterococcus (VRE), and other Gram-negative organisms.
Limited access to hand hygiene facilities, such as sinks and hand sanitiser stations, can hinder compliance. Patients and aged care residents with mobility issues may find it challenging to reach these facilities, leading to lower rates of hand hygiene. Lack of awareness about the importance of hand hygiene or forgetfulness can also contribute to poor compliance.
Whilst healthcare workers often believe that they offer patients and residents the opportunity to wash their hands, reporting and perceptions from patients, as well as direct observations suggests that this does not always happen as often as thought by the healthcare worker.5,6
To promote hand hygiene with patients and residents, healthcare facilities can implement various strategies. Providing easy access to hand hygiene facilities is crucial. Providing easy-to-access options such as Antibacterial Hand Wipes as a part of a meal tray or placing sinks and alcohol-based hand sanitisers in convenient locations encourages everyone to clean their hands regularly. Educating patients and residents about the importance of hand hygiene and demonstrating proper handwashing techniques can also be effective. Using visual aids, such as posters, can serve as reminders for patients and residents to clean their hands.7 Healthcare providers should lead by example and practice good hand hygiene themselves, reinforcing the importance of this behaviour to those under their care.

Implementation of a patient hand hygiene bundle in one study showed an increase of hand hygiene compliance from 13% to 60% after implementation.7 This bundle included:
- Multipack of hand wipes provided to each patient
- An information card advising patients when to perform hand hygiene with the hand wipe pack
- Staff protocol for patient hand hygiene advising opportunities for staff support to encourage patients to clean their hands
Patient and resident hand hygiene is a vital component of infection prevention in healthcare settings. By providing access to hand hygiene facilities, educating patients and residents about the importance of hand hygiene, and implementing hand hygiene options like hand wipes, healthcare facilities can improve hand hygiene compliance. Ultimately, these efforts contribute to a safer and healthier healthcare environment for patients, aged care residents, healthcare workers, and visitors alike.
Join our Stay a Step Ahead IPC Winter Campaign to learn more about effective infection control strategies and enter the IPC Hot Tips Competition for the chance to win exciting prizes.
References
1. World Health Organisation. (2022). Hand Hygiene. World Health Organisation. https://www.who.int/teams/integrated-health-services/infection-prevention-control/hand-hygiene
2. National Health and Medical Research Council (NHMRC). (2019). Australian Guidelines for the Prevention and Control of Infection in Healthcare. Australian Commission on Safety and Quality in Healthcare.
3. Istenes, N., Bingham, J., Hazelett, S., Fleming, E., & Kirk, J. (2013). Patients’ potential role in the transmission of health care-associated infections: Prevalence of contamination with bacterial pathogens and patient attitudes toward hand hygiene. American Journal of Infection Control, 41(9), 793–798. https://doi.org/10.1016/j.ajic.2012.11.012
4. Okada, J., Yamamizu, Y., & Fukai, K. (2016). Effectiveness of hand hygiene depends on the patient’s health condition and care environment. Japan Journal of Nursing Science, 13(4), 413–423. https://doi.org/10.1111/jjns.12122
5. Burnett, E. (2009). Perceptions, attitudes, and behavior towards patient hand hygiene. American Journal of Infection Control, 37(8), 638–642. https://doi.org/10.1016/j.ajic.2009.04.281
6. Sunkesula, V. C., Knighton, S., Zabarsky, T. F., Kundrapu, S., Higgins, P. A., & Donskey, C. J. (2015). Four Moments for Patient Hand Hygiene: A Patient-Centered, Provider-Facilitated Model to Improve Patient Hand Hygiene. Infection Control & Hospital Epidemiology, 36(8), 986–989. https://doi.org/10.1017/ice.2015.78
7. Loveday, H., Tingle, A., & Wilson, J. (2020). Using a multi-modal Strategy to Improve Patient Hand Hygiene. American Journal of Infection Control, 49(6). https://doi.org/10.1016/j.ajic.2020.12.011
SHARE THIS ARTICLE
Tags
Latest News
Can patient and resident hand hygiene be part of the solution to preventing infections?
The importance of practising proper hand hygiene is widely considered…
Confronting the hidden threat of C. diff
The power of effective surface decontamination The hidden threat of…
Reflections and learnings from International Infection Prevention Week (IIPW)
International Infection Prevention Week shines a spotlight on the crucial…
Access to patient isolation rooms matters
Infection prevention and control is complex and incorporates a whole…